
Rotator Cuff Tears: Common findings on scans — not always the cause of shoulder pain -
Understanding what a rotator cuff tear really means in clinical practice
Get WISE - Get WELL
- Get ON
The rotator cuff is a group of muscles and tendons that help control shoulder movement and stability. Changes within these tissues usually develop gradually over time rather than as a single injury. Because of this, the presence of a tear needs to be interpreted carefully and always in the context of symptoms, function, and clinical assessment — not in isolation.
Understanding what a rotator cuff tear actually means, and just as importantly what it does not mean, is key to making sensible decisions about treatment. Effective management focuses on how the shoulder behaves and what it can do, rather than relying on scan findings alone.
This article explains:
-
Key Facts First
-
Bones of the Shoulder
-
Muscles of the Rotator Cuff
-
The Supraspinatus
-
The Subscapularis
-
The Infraspinatus
-
Teres Minor
-
What Are Rotator Cuff Tears?
-
How Are Rotator Cuff Tears Classified?
-
The Most Common Practical Classifications
-
Causes of Rotator Cuff Tears
-
Symptoms of Rotator Cuff Tears
-
Diagnosis of Rotator Cuff Tears
-
Treatment Options for Rotator Cuff Tears
-
Recovery Timescales for Rotator Cuff Tears
-
Summary
-
Rotator Cuff FAQ's
Key Facts First
Rotator cuff tears are often explained poorly.
They’re either oversimplified — “you’ve torn it, that’s the problem” — or described in a way that feels technical and overwhelming.
This is a complex topic.
My aim here is to give you the detail you actually need to understand your shoulder properly — without it becoming confusing or unreadable. If you take this step by step, it will make sense.
Before we go into depth, here are the key things most people are not told:
-
A rotator cuff tear does not automatically cause pain
-
Many people over 50 have tears and no symptoms
-
Strength loss is often more important than scan findings
-
Most tears can be managed without surgery
-
Imaging is not always necessary
-
Large traumatic tears are different and need early assessment
-
Rehabilitation is usually the first-line treatment
Now let’s break it down properly.
Bones of the Shoulder
Before focusing specifically on the rotator cuff, it helps to understand the bones that form the foundation of the joint. The shoulder is a ball-and-socket joint made up of three bones: the scapula (shoulder blade), clavicle (collarbone), and humerus (upper arm bone). The scapula provides a shallow socket (the glenoid), into which the rounded head of the humerus fits. If you'd like to explore this in more depth, you can visit the full shoulder anatomy guide for a broader overview.

Muscles of the Rotator Cuff
The rotator cuff is a group of four deep muscles and their tendons that surround the shoulder joint. Working together, they play a vital role in stabilising the ball of the humerus within the shallow socket of the scapula. While larger muscles like the deltoid generate power, the rotator cuff provides the fine control and joint security needed for smooth, pain-free movement — especially during lifting, rotation, or reaching overhead. Each muscle has a distinct function, which becomes especially important when understanding shoulder injuries or planning rehabilitation.
If the rotator cuff is not functioning well, the shoulder can become painful, weak, or mechanically inefficient.

The Supraspinatus
The supraspinatus is the most commonly injured of the four rotator cuff muscles. It sits at the top of the shoulder ( originating from the supraspinous fossa, the concave surface above the spine of the scapula and passing under the acromion before attaching to the superior facet of the greater tubercle of the humerus) and helps lift your arm away from your body. Its unique path through the narrow subacromial space makes it particularly vulnerable to overload and compression during movement.


Clinical Relevance:
-
The supraspinatus tendon is the most frequently injured structure in rotator cuff pathology — commonly affected by tendinopathy, partial-thickness tears, or full-thickness tears.
-
It is particularly susceptible to impingement beneath the acromion (the bony outcrop of the shoulder blade), especially in individuals with altered shoulder mechanics or structural narrowing of the subacromial space.
-
Weakness or dysfunction of the supraspinatus can cause difficulty initiating abduction, a “painful arc” (typically between 60–120° of abduction), and a sense of instability or weakness during overhead activity.
-
Imaging (e.g. ultrasound or MRI) often focuses on this tendon when assessing rotator cuff injuries, as it is a common site of degeneration with age or repetitive use.
Primary Function:
-
The supraspinatus is responsible for initiating abduction of the shoulder, lifting the arm away from the body for the first 15–20 degrees of movement.
-
Beyond this initial phase, the deltoid muscle becomes the primary abductor in a graduated fashion until about 90 degrees, where the supraspinatus is no longer really active.
Additional Roles:
-
It plays a crucial role in stabilising the humeral head within the glenoid socket during all shoulder movements.
-
Works in coordination with the other rotator cuff muscles to provide dynamic control (movement through a certain range, not stationary) of the joint and prevent excessive translation of the humerus.
The Subscapularis
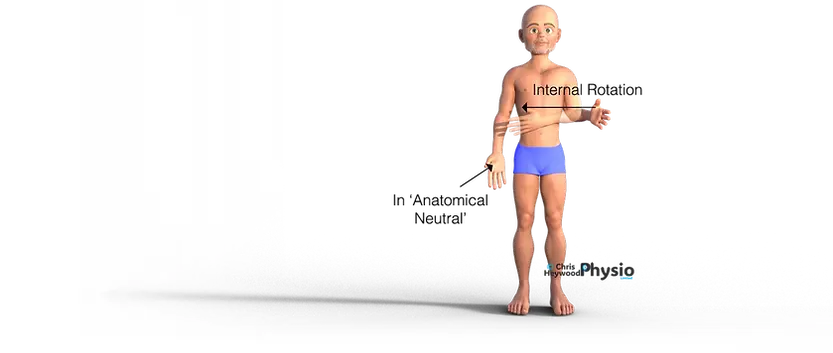
The subscapularis is the largest and strongest of the four rotator cuff muscles. It originates from the subscapular fossa on the front surface of the scapula (shoulder blade) and travels across the front of the shoulder joint to insert onto the lesser tubercle of the humerus. Its position at the front of the joint allows it to play a unique role in both shoulder movement and anterior joint stability.
Primary Function:
-
The subscapularis is the main internal rotator of the shoulder. It allows you to rotate your arm inwards — a movement used for actions like placing your hand on your stomach, reaching across your body, or tucking in your shirt.
-
It also assists with adduction of the arm, particularly when the arm is elevated.
Additional Roles:
-
This muscle acts as a dynamic stabiliser of the shoulder joint, helping to keep the humeral head securely positioned in the glenoid socket during arm movements.
-
Because of its location, it also resists anterior translation of the humeral head, helping to prevent the shoulder from slipping forward — particularly important in positions of external rotation or elevation.
Clinical Relevance:
-
Subscapularis injuries are less common than supraspinatus tears but still significant. Damage to this muscle can cause weakness in internal rotation, anterior (front) shoulder pain, and difficulty with functional tasks like reaching behind your back or fastening clothing.
-
Tears are often associated with trauma, degenerative changes, or as part of massive rotator cuff tears.
-
It’s also a key structure to assess following shoulder dislocations, particularly in older adults.
The Infraspinatus
The infraspinatus is a thick, triangular muscle that lies on the back of the scapula, just below the spine of the shoulder blade. It originates from the infraspinous fossa and attaches to the middle facet of the greater tubercle of the humerus. Alongside the teres minor, it plays a vital role in external (lateral) rotation of the shoulder and contributes significantly to joint stability during movement.
Primary Function:
-
The infraspinatus is one of the primary external rotators of the shoulder. It allows you to rotate your arm outward, such as when reaching to put on a jacket, throwing, or preparing for a tennis backhand.
-
Also assists with horizontal abduction when the arm is lifted to shoulder height.

Additional Roles:
-
Like all rotator cuff muscles, the infraspinatus helps to compress the humeral head into the glenoid cavity, ensuring the joint remains centred during movement.
-
It is particularly important during overhead or high-velocity activities, where it provides fine-tuned control and dynamic joint stability.
Clinical Relevance:
-
The infraspinatus is often affected in overhead athletes (e.g. tennis players, cricketers, swimmers) due to repetitive external rotation demands.
-
It may become strained, overloaded, or affected by tendinopathy, especially in conjunction with supraspinatus pathology.
-
Tears of the infraspinatus can lead to weakness in external rotation, posterior (back)shoulder pain, and sometimes a loss of control or power when reaching outward or backward.
-
Chronic (>12 weeks) injuries can contribute to posterior shoulder tightness, altered scapular mechanics, and symptoms commonly referred to as posterior impingement.
Teres Minor
The teres minor is the smallest of the four rotator cuff muscles, but it plays an important role in shoulder stability and control. It originates from the upper two-thirds of the lateral border of the scapula and inserts onto the inferior facet of the greater tubercle of the humerus, just below the insertion of the infraspinatus.
Primary Function:
-
Like the infraspinatus, the teres minor contributes to external rotation of the shoulder, particularly when the arm is abducted.
-
It plays a supportive role during activities that involve rotation, deceleration, or controlled lowering of the arm.Weakness in the teres minor can reduce external rotation strength and cause difficulty with controlled arm positioning.

Additional Roles:
-
Teres minor is involved in stabilising the humeral head within the glenoid socket, especially during rotational movements and overhead activity.
-
Often functions as part of a unit with the infraspinatus, but may contribute more during late-phase abduction and fine-tuned rotational control.
Clinical Relevance:
-
Isolated injuries to the teres minor are uncommon, but it may be affected in larger posterior cuff tears or in chronic degenerative rotator cuff pathology.
-
In some cases of massive cuff tears (involving supraspinatus and infraspinatus), the teres minor may be the only remaining external rotator — making it crucial for maintaining some degree of shoulder function.
-
This muscle is also assessed in relation to quadrilateral space syndrome, where it may become compressed along with the axillary nerve, leading to weakness or atrophy.
-
Weakness in the teres minor can reduce external rotation strength and cause difficulty with controlled arm positioning.
What Are Rotator Cuff Tears?
A rotator cuff tear refers to a disruption of one or more of the tendons that attach the rotator cuff muscles to the upper arm bone (humerus).
The term “tear” can sound dramatic — but it does not always mean the tendon has completely snapped.
Tears vary widely in:
-
Depth
-
Size
-
Location
-
Chronicity (how long they have been present)
-
Functional impact
Some are small and stable. Some are large and traumatic. Some cause weakness. Some cause no symptoms at all.
This variation is why careful assessment matters.
How Are Rotator Cuff Tears Classified?
This is where things become slightly more complex.
There are multiple classification systems used in research and surgery to describe rotator cuff tears. However, no single system has been universally adopted as the global gold standard.
Different systems classify tears based on:
-
Thickness (partial vs full)
-
Size (small, medium, large, massive)
-
Shape (crescent, U-shaped, L-shaped)
-
Tendon involvement (which tendon is affected)
-
Retraction (how far the tendon has pulled back)
-
Muscle quality (fatty degeneration on imaging)
These systems are useful in surgical planning and research — but for patients, the most important factors are usually:
-
How strong the shoulder is
-
How much function is limited
-
Whether the tear occurred suddenly or gradually
A classification label on its own does not determine treatment.
The Most Common Practical Classifications
For clarity, most clinicians simplify tears into the following broad categories:
1. Partial-Thickness Tears
The tendon is damaged but not completely detached from the bone.
These are common and frequently managed conservatively.
2. Full-Thickness Tears
The tendon is completely disrupted.
These may still vary greatly in size and impact.
3. Small, Medium, Large, or Massive Tears
This refers to the measured size of the tear.
Larger tears are more likely to produce measurable weakness — but size alone does not predict pain.
4. Traumatic vs Degenerative Tears
Traumatic tears
-
Occur suddenly
-
Often cause immediate weakness
-
May require earlier surgical consideration
Degenerative tears
-
Develop gradually
-
Common with ageing
-
Frequently manageable without surgery
Why Classification Matters — But Only to a Point
Classification systems help describe anatomy. They do not automatically dictate treatment.
Two people with the same-sized tear may have very different:
-
Pain levels
-
Strength
-
Functional capacity
-
Recovery potential
This is why clinical assessment remains more important than the label applied to the tear.
Causes of Rotator Cuff Tears
A rotator cuff tear occurs when one or more of the rotator cuff tendons become partially or completely disrupted.
This can happen:
-
Suddenly, after trauma (a fall, heavy lift, or shoulder dislocation
-
Gradually, over time due to age-related tendon changes
-
Through repeated loading or long-term mechanical stress
Tears are commonly associated with shoulder pain and weakness — particularly in middle-aged and older adults — but the relationship between a tear and symptoms is not straightforward.imaging alone.
There are almost always more benefits than drawbacks to staying fit and active, and as more people take this advice on board, we’re seeing new sports and activities gain popularity.
In my own practice, I’ve noticed a marked increase in walking football–related injuries over the last five years. It reminds me a bit of netball — arguably the most contact “non-contact” sport out there!

The combination of natural age-related changes — such as reduced balance, slower reflexes, and stiffer joints — with a renewed outlet for competitiveness often leads to falls onto an outstretched arm. Unsurprisingly, this is a common mechanism for shoulder injuries, including rotator cuff tears.
-
Degeneration: As we get older, the tendons in our shoulder naturally weaken — just like the tread on a tyre gradually wears down. This kind of age-related degeneration is the most common reason for a rotator cuff tear, especially in people over 60. An example of this may be that you haven’t had a fall or injury, but over the years you’ve developed a dull ache in your shoulder, especially at night. You might even have a tear and not know it, because the body has slowly adapted over time.
-
Repetitive Actions: Doing the same shoulder motion repeatedly — particularly overhead — can gradually irritate or damage the rotator cuff. This is common in both sports and everyday tasks. A relatable example could be that you play tennis a few times a week, swim regularly, or work as a decorator or hairdresser. Even reaching up to hang washing, paint a ceiling, or lift boxes onto high shelves can eventually strain the tendon enough to cause a tear.
-
Bone Spurs: In some people, small bony overgrowths (called spurs) develop around the shoulder joint. These can rub against the tendon every time you move your arm, gradually wearing it down — like a frayed rope over a sharp edge. We see patients that deny ever injuring their shoulder, but they’ve had years of limited movement and now their arm feels weak or painful when reaching overhead — particularly when putting things in cupboards or lifting something to an overhead locker.
Symptoms of Rotator Cuff Tears
Rotator cuff tears can present in different ways — and not everyone experiences the same symptoms. The way a tear behaves often depends on how it developed, how large it is, and how your shoulder is used day-to-day.
Even with a confirmed tear, some people have only mild discomfort, while others notice significant pain and weakness. Importantly, a tear do
Here are the most commonly reported symptoms:
Pain in the Shoulder
-
A deep, aching pain felt over the top and outer side of the shoulder and upper arm is common.
-
Pain may be worse at night, especially when lying on the affected side, or when trying to sleep.
-
The pain can be a dull ache, sharp with certain movements, or both.
Some people describe it as a general discomfort that seems to increase with use or specific positions — for example reaching overhead or behind the back.
Weakness
Weakness is often a clue that the rotator cuff’s ability to generate force is compromised:
-
Difficulty lifting objects, carrying everyday items, or doing tasks that were once easy.
-
A sense that the arm just “won’t do what it used to” — especially with lifting or reaching.
Weakness tends to become more noticeable with overhead activities or when trying to control movement rather than just passively lifting the arm.
Altered Movement or Stiffness
-
Some people feel that their shoulder does not move as smoothly as normal, or feels “stuck” in certain positions.
-
You might notice a catching, clicking, or grating sensation during movement.
-
Reaching behind the back (e.g., to fasten a bra, reach into a rear pocket, or put on a coat) may be difficult or limited.
Range of motion can be reduced, not just because of pain but because muscle control and coordination are affected.
Activity-Related Irritation
The shoulder might feel fine at rest, but symptoms can be triggered or worsened by specific actions such as:
-
Repeated overhead work
-
Reaching up or behind
-
Throwing, lifting, or pushing heavy objects
These provoke symptoms because they load the rotator cuff tendons and require coordinated muscle activity.
Sudden Weakness After Trauma
In traumatic tears — such as from a fall or forceful pull — people often report:
-
Sudden, intense pain at the time of injury
-
Immediate inability to lift the arm or a marked loss of strength
This pattern is different from the gradual discomfort of chronic, degenerative tears and may warrant more urgent assessment.
What Symptoms Do Not Always Mean
Not every rotator cuff tear causes:
-
Severe pain
-
Complete loss of function
-
A dramatic limp or “dead arm”
Some people function quite well despite sizable tears — especially if other muscles compensate. This is why it’s often more useful to look at functional impact than just pain intensity.
When Symptoms Suggest Something Else
Though rotator cuff tears have characteristic symptoms, other shoulder conditions can mimic them. For example:
-
Shoulder impingement typically causes pain at the top and outside of the shoulder, worse with overhead movement.
-
Biceps tendon issues can refer pain down the arm.
-
Arthritis often limits range of motion with pain at rest or first thing in the morning.
-
Nerve-related pain may cause pins-and-needles or numbness rather than muscle weakness.
If you notice unfamiliar sensations like numbness, burning, or radiating numbness beyond the shoulder distribution, that may suggest involvement of a nerve or cervical spine issue rather than a pure rotator cuff tear.
Summary — What Most People Experience
In simple terms, symptoms often fall into three broad buckets:
-
Pain in the shoulder and upper arm
-
Weakness with lifting or reaching
-
Altered movement or stiffness
Not all tears will cause all three — and some tears cause minimal or no symptoms at all. Functional impact and symptom irritability are usually more important than imaging signs alone.
Diagnosis of Rotator Cuff Tears
Diagnosing a rotator cuff tear is not simply a case of ordering a scan. It begins with a detailed clinical assessment.
The goal is to understand:
-
How the symptoms developed
-
How the shoulder behaves under load
-
Whether strength is measurably reduced
-
How movement quality has changed
-
Whether the presentation fits a traumatic or degenerative pattern
The diagnosis is built from this bigger picture — not from imaging alone.
Step 1: The History
Your story matters. A gradual onset of shoulder pain with increasing irritation under load suggests a different mechanism from a sudden loss of strength after a fall.
Key questions include:
-
Did symptoms begin after a specific injury?
-
Has strength noticeably reduced?
-
Is there night pain?
-
Has function changed?
-
Is the shoulder progressively worsening or stable?
Patterns often provide more diagnostic value than a single test.
Step 2: Physical Examination
A structured shoulder examination typically assesses:
Range of Movement
Is movement restricted due to pain, stiffness, or weakness?
True stiffness suggests joint involvement.
Painful but preserved range often suggests tendon irritation.
Marked weakness during movement raises suspicion of structural disruption.
Strength Testing
Specific resisted movements help identify which tendon may be involved.
The key clinical question is not simply “is it painful?” but:
-
Is there true strength loss?
-
Is the weakness pain-limited or power-limited?
-
Is there asymmetry compared to the other side?
Significant objective weakness, particularly after trauma, increases suspicion of a larger tear.
Load Response
How does the shoulder tolerate controlled loading?
Sometimes pain is high but strength remains largely intact.
Other times pain is modest but force production is clearly reduced.
Understanding irritability helps guide management decisions.
Step 3: When Is Imaging Helpful?
Imaging can provide structural detail, but it does not replace examination.
Ultrasound and MRI are commonly used to visualise:
-
Tendon continuity
-
Tear size
-
Retraction
-
Muscle quality
However, imaging is usually considered when:
-
There is significant traumatic onset
-
Strength loss is substantial
-
Symptoms fail to improve with appropriate rehabilitation
-
Surgical referral is being considered
In many gradual-onset cases, early imaging does not change management.
The clinical findings determine whether imaging will meaningfully alter the treatment pathway.
Diagnostic Uncertainty Is Normal
Shoulders are complex.
Several conditions can present with similar symptoms, including:
-
Rotator cuff tendinopathy
-
Subacromial pain syndrome
-
Biceps tendon irritation
-
Glenohumeral joint pathology
-
Referred cervical spine pain
This overlap is why diagnosis is rarely based on a single special test or scan result.
It is the consistency of findings — across history, movement, strength and response to load — that builds diagnostic confidence.
What Matters Most in Practice
From a practical perspective, diagnosis is less about attaching a label and more about answering three key questions:
-
Is there meaningful strength loss?
-
Is the shoulder progressively deteriorating?
-
Does the presentation suggest a tear that would change management?
If the answer to those is no, conservative rehabilitation is often appropriate regardless of scan findings.
A Final Word on Diagnosis
A rotator cuff tear is a structural description. A diagnosis should describe how the shoulder is functioning. That distinction matters — because management decisions depend on function, not just anatomy.
Treatment Options for Rotator Cuff Tears
Treatment depends on context.
Not all tears require the same approach. Management is influenced by:
-
Age
-
Activity demands
-
Tear type and size
-
Degree of strength loss
-
Symptom irritability
-
Whether the onset was traumatic or gradual
For most people, conservative management is the first-line approach.
Conservative (Non-Surgical) Management
The majority of rotator cuff tears — particularly degenerative ones — can be managed without surgery.
Rehabilitation is not simply about “doing exercises.”
It is a staged process that restores load tolerance and strength.
Stage 1 – Settle Irritability
When the shoulder is painful and reactive, the priority is control — not aggressive strengthening.
This stage focuses on:
-
Modifying aggravating loads
-
Maintaining gentle movement
-
Avoiding prolonged immobilisation
-
Reducing night pain triggers
-
Preserving basic function
-
Complete rest is rarely helpful. Equally, repeatedly pushing into pain can prolong irritability. The aim is to calm the shoulder without allowing deconditioning.
Stage 2 – Restore Strength and Control
This is the most important phase. Rotator cuff tears affect force production and dynamic stability. Strength deficits often persist unless specifically addressed.
Rehabilitation here involves:
-
Progressive resistance loading
-
Targeted rotator cuff strengthening
-
Scapular control work
-
Gradual exposure to previously painful movements
The key principle is progressive overload — carefully increasing demand in a controlled manner. Pain during this stage is not automatically harmful, but uncontrolled flare-ups should be avoided.
Strength improvements can occur even in the presence of structural tears.
Stage 3 – Rebuild Functional Capacity
Once strength improves, the focus shifts to real-world demands.
This may include:
-
Overhead endurance
-
Lifting tolerance
-
Manual work tasks
-
Sport-specific drills
-
Repeated load exposure
This stage determines whether rehabilitation has truly restored function — not just reduced pain.
When Is Surgery Considered?
Surgery is not the default solution.
It may be considered when:
-
There is a large acute traumatic tear
-
Significant weakness persists
-
Function remains severely limited despite rehabilitation
-
There is progressive deterioration
-
The individual has high physical demands
Surgical repair aims to reattach the tendon to bone however, surgery does not remove the need for rehabilitation. Post-operative recovery typically involves several months of structured rehab.
Outcomes vary depending on:
-
Tear size
-
Tissue quality
-
Age
-
Muscle degeneration
-
Compliance with rehabilitation
It is important to recognise that surgery addresses structure — but function still needs to be rebuilt.
Do Tears Heal?
This is a common and understandable question. Small partial tears may remain stable for long periods. Some tears do not “heal” structurally but become functionally well-tolerated.
The body can adapt. Strength can improve. Pain can reduce. Function can return.
Structural integrity and symptom resolution are not always the same thing.
Prognosis
Prognosis depends on:
-
Tear type
-
Chronicity
-
Muscle quality
-
Load demands
-
Rehabilitation quality
In many degenerative cases:
-
Pain improves before strength fully returns
-
Progress is gradual rather than linear
-
Flare-ups can occur but do not necessarily indicate worsening damage
In traumatic cases with significant weakness, earlier intervention may alter prognosis. The key determinant is how well the shoulder regains strength and load tolerance.
A Practical Management Framework
When deciding on management, three core questions guide the pathway:
-
Is strength meaningfully reduced?
-
Is function significantly impaired?
-
Is the presentation likely to worsen without structural repair?
If not, structured rehabilitation is usually appropriate. If yes, surgical opinion may be warranted.
Final Perspective
A rotator cuff tear is a structural finding. Management decisions should be based on:
-
Functional impact
-
Strength capacity
-
Load tolerance
-
Individual goals
-
Treatment is not about fixing a scan. It is about restoring shoulder performance.
Recovery Timescales for Rotator Cuff Tears
One of the most common questions is:
“How long will this take to recover?”
The honest answer is: it depends on the type of tear, the severity of weakness, and how the shoulder responds to rehabilitation.
However, we can outline broad patterns.
Gradual (Degenerative) Tears Managed Conservatively
For many people with gradual-onset symptoms:
-
Pain often begins to improve within 4–8 weeks of structured rehabilitation.
-
Strength gains typically take 8–16 weeks.
-
Full functional confidence may take 3–6 months, depending on demands.
Improvement is usually gradual rather than dramatic.
Flare-ups can occur, particularly if load is increased too quickly — but these do not automatically mean the tear has worsened. The key variable is progressive strength restoration.
Partial-Thickness Tears
When weakness is modest and the tear is partial:
-
Symptom reduction may occur within 6–12 weeks.
-
Strength improvements may continue for several months.
-
Many individuals regain high levels of function without surgical repair.
Structural healing is less important than functional improvement.
Large or Traumatic Tears (Non-Surgical Management)
If the tear occurred after trauma but is managed conservatively:
-
Early progress is often slower.
-
Strength recovery may take 3–6 months or longer.
-
Functional adaptation may continue over 6–12 months.
In these cases, expectations must be realistic and progression carefully staged.
Post-Surgical Recovery
If surgical repair is performed, recovery follows a more structured timeline:
-
First 4–6 weeks: Protection phase (limited active movement)
-
6–12 weeks: Gradual restoration of movement
-
3–6 months: Progressive strengthening
-
6+ months: Higher-level function and return to demanding activity
Return to heavy manual work or sport may take 6–9 months, sometimes longer. Surgery addresses tendon attachment — but rebuilding strength and coordination takes time.
What Influences Recovery Speed?
Recovery is influenced by:
-
Tear size
-
Muscle quality
-
Age
-
Baseline strength
-
Adherence to rehabilitation
-
Load demands at work or sport
-
Irritability levels
Two people with similar scans may recover at very different rates.
Pain vs Strength Recovery
It is important to understand that:
-
Pain often improves before strength returns.
-
Feeling “better” does not mean the shoulder is fully rehabilitated.
-
Stopping rehab too early increases recurrence risk.
Long-term outcomes depend more on strength restoration than short-term pain reduction.
A Realistic Expectation
For most non-surgical cases:
-
Expect noticeable improvement within 6–12 weeks.
-
Expect strength rebuilding over 3–6 months.
-
Expect gradual confidence restoration rather than instant change.
Recovery is rarely linear — but steady progress is typical with appropriate management.
Summary - Key Takeaways
Rotator cuff tears are a common shoulder condition that can be both confusing and misunderstood. This page explains what a tear really means in clinical practice — focusing on how the shoulder functions, not just what a scan shows.
The rotator cuff is a group of four deep muscles and their tendons that stabilise and control the shoulder. Tears can happen suddenly from trauma or develop gradually over time due to degeneration and repetitive loading.
A key principle throughout this page is that a rotator cuff tear does not always cause pain. Especially with ageing, many people have tears on imaging and no symptoms at all. This emphasises an important point: the presence of a tear on a scan doesn’t automatically explain pain or dictate treatment.
Rotator cuff tears are categorised in several ways, but no single classification system is universally adopted. Clinically relevant distinctions include:
-
Partial vs full–thickness tears
-
Size (small, medium, large, massive)
-
Traumatic vs degenerative tears
However, classification alone does not determine management — the focus is always on function, strength, and symptom behavior.
The page then explores common presentations:
-
Pain, often a deep ache that can be worse at night or with movement
-
Weakness, noticeable in lifting or reaching tasks
-
Altered movement or stiffness, affecting how the shoulder feels and performs
-
Activity-related irritability, where symptoms are triggered by specific loads
It emphasises that symptoms alone are not diagnostic. Diagnosis starts with a detailed clinical assessment — history, movement analysis, and strength testing — with imaging used selectively when it will truly influence management.
In the treatment section, the page outlines a staged approach:
-
Settle irritability and manage symptoms without deconditioning
-
Restore strength and control through progressive, targeted rehabilitation
-
Rebuild functional capacity for real-world tasks
Most tears, especially degenerative ones, are managed conservatively with rehabilitation as the first line. Surgery is considered in specific situations — for example, large traumatic tears with marked weakness or when conservative care hasn’t restored function.
A dedicated section on recovery timescales clarifies expectations:
-
Symptom improvement may begin within weeks
-
Strength gains typically take months
-
Full functional recovery, especially after surgery, can extend over several months
The page reinforces that recovery varies widely and is influenced by tear characteristics, baseline strength, load demands, and rehabilitation quality.
Finally, the summary emphasises that a rotator cuff tear is a structural description, not a definitive diagnosis.
Management should be guided by functional impact and clinical reasoning rather than imaging alone. The overall aim is to help readers make informed decisions about their shoulder — with clear, honest guidance.
Educational Notice
This content is intended for educational guidance only and reflects current evidence and clinical reasoning at the time of publication. It does not replace individual assessment, diagnosis, or treatment provided by your healthcare practitioner. Management decisions should always be based on personalised clinical evaluation.
Feel Free To Share
There is a great deal of misinformation and oversimplified advice online regarding musculoskeletal and spinal conditions. If you have found this page helpful, you are very welcome to share it with anyone who may benefit from clear, evidence-informed information.
Please share the page in full via direct link. Reproduction, copying, or republishing of the written content or images without permission is not permitted. Producing accurate educational material of this depth takes significant time, clinical experience, and ongoing review — and I choose to keep it freely accessible for the benefit of patients and healthcare professionals.
Responsible sharing is genuinely appreciated.
Rotator Cuff Tear FAQs
1. Can a rotator cuff tear heal on its own?
Small or partial tears may remain stable for years.
Some tears do not structurally “heal,” but the shoulder can become strong and functional despite the tear.
In many cases, symptom improvement and strength restoration are more important than structural repair.
2. Do I need surgery for a rotator cuff tear?
Not necessarily.
Most degenerative tears are managed successfully with structured rehabilitation.
Surgery is typically considered when there is:
-
A large traumatic tear
-
Significant and persistent weakness
-
Failure to improve with appropriate conservative care
-
The decision is based on function and demand — not just scan findings.
3. Is it safe to exercise with a rotator cuff tear?
Yes — in most cases, exercise is the primary treatment.
Loading must be progressive and appropriate to irritability levels, but avoiding movement entirely often delays recovery.
Rehabilitation focuses on restoring strength, control and load tolerance.
4. Why does my scan show a tear if my pain isn’t severe?
Rotator cuff tears are common, particularly with increasing age.
Structural findings on imaging do not always correlate with pain levels.
Assessment focuses on how the shoulder functions — not just what appears on a scan.
5. How long does recovery take?
Recovery varies depending on tear type and severity.
For non-surgical cases:
-
Pain often improves within 6–12 weeks
-
Strength rebuilding can take 3–6 months
After surgery, rehabilitation commonly lasts several months. Progress is gradual rather than immediate.
6. Will the tear get worse if I don’t have surgery?
Not always. Many degenerative tears remain stable for years.
Progression risk depends on tear size, muscle quality and loading demands. Monitoring strength and function is often more important than repeated imaging.
8. What does physiotherapy focus on for rotator cuff tears?
Physiotherapy focuses on restoring shoulder strength, control, and load tolerance rather than trying to “fix” the tear itself. Treatment aims to improve how the shoulder functions in daily life, work, or sport, using progressive exercise and activity modification.
9. Can injections fix a rotator cuff tear?
Injections do not repair a tear. They may reduce pain in some cases and allow rehabilitation to progress, but they are not a long-term solution and should not be used in isolation. Their role should be considered carefully within an overall management plan.
10. What is the long-term outlook with a rotator cuff tear?
The long-term outlook is generally good. Many people regain function and manage symptoms well with appropriate rehabilitation, even when a tear is present. The goal is a strong, reliable shoulder that supports your activities — not necessarily a perfect scan.
Why You Should Choose Chris Heywood Physio
The most important thing when seeking help is finding a practitioner you trust—someone who is honest, responsible, and clear about your diagnosis, the treatment you really need, and whether any follow-up appointments are necessary.
I’m not here to poach you from another therapist, but if you’re looking for a new physiotherapist in Northamptonshire or simply want a second opinion, here’s why many people choose to work with me (read my reviews):
Over 25 Years of Experience & Proven Expertise
With 25+ years of hands-on physiotherapy experience, I’ve built a trusted reputation for clinical excellence and evidence-based care. My approach combines proven techniques with the latest research, so you can feel confident you’re in safe, skilled hands.
Longer Appointments for Better Results
No two people—or injuries—are the same. That’s why I offer 60-minute one-to-one sessions, giving us time to:
-
Thoroughly assess your condition
-
Provide focused, effective treatment
-
Explain what’s really going on in a clear, simple way
Your treatment plan is tailored specifically to you, aiming for long-term results, not just temporary relief.
Honest Advice & Support You Can Trust
I’ll always tell you what’s best for you—even if that means you need fewer sessions, not more. My goal is your recovery and wellbeing, not keeping you coming back unnecessarily. I have low overheads nowadays and I do not have pre-set management targets to maximise patient 'average session per condition' (yes it does happen commonly and I hate it with a passion - read my article here)
Helping You Take Control of Your Recovery
I believe the best outcomes happen when you understand your body. I’ll explain your condition clearly, give you practical tools for self-management, and step in with expert hands-on treatment when it’s genuinely needed.
Looking for a physiotherapist who values honesty, expertise, and your long-term health?
Book an appointment today and take the first step towards feeling better.
Contact Info
On a Monday and Tuesday I work as a advance musculoskeletal specialist in primary care but I can still be contacted for enquiries. You are welcome to call but it is often faster for me to reply via an email or watsapp message, simply as my phone will be on silent in clinic. Either way, I will reply as soon as possible, which in the week, is almost always on the same day at the latest.

Clinic Opening Hours
** Please note that online sessions and Aquatic sessions be arranged outside of normal clinical hours on request.**
Sat -Sun
Closed
0900 - 1430
Closed - FCP
Weds - Fri
Mon - Tues










