
De Quervain’s Tenosynovitis
Pain on the thumb side of the wrist caused by irritation of the first dorsal compartment
Get WISE - Get WELL
- Get ON
De Quervain’s tenosynovitis is a condition affecting two thumb tendons — the abductor pollicis longus (APL) and extensor pollicis brevis (EPB) — as they pass through a narrow fibro-osseous tunnel on the thumb side of the wrist known as the first dorsal compartment.
When these tendons are repeatedly loaded or compressed within this confined space, their ability to glide smoothly becomes impaired. This leads to pain along the radial (thumb) side of the wrist, particularly during gripping, lifting, twisting, or repetitive thumb movement.
Although often labelled as a purely inflammatory condition, many cases involve structural thickening of the tendon sheath and mechanical restriction rather than acute inflammation alone. The underlying problem is friction within a limited space.
This article explains the anatomy, why it develops, how it differs from thumb arthritis and nerve conditions, and what evidence-based management looks like:
-
Anatomy Related to De Quervain's Tenosynovitis
-
The First Dorsal Compartment
-
Tendon Sheath Mechanics
-
Clinical History and Symptom Behaviour
-
Physical Examination
-
The Role of Nerve Conduction Studies and Imaging
-
Treatment and Management of De Quervain’s Tenosynovitis
-
Summary
-
De Quervain's Tenosynovitis FAQ's
Anatomy Related to De Quervain's Tenosynovitis
The structure of the wrist and hand provides both mobility and stability — a balance that allows precision grip, power grip, and fine motor control.
The wrist joint itself is formed by the distal ends of the radius and ulna and a complex arrangement of eight small carpal bones. These carpal bones form two rows and articulate with the forearm to create the radiocarpal joint, which allows flexion, extension, radial deviation and ulnar deviation.

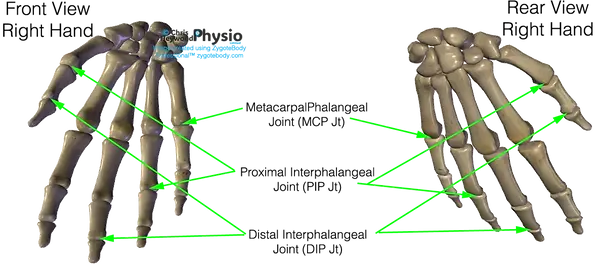
From the carpus, the hand extends into five metacarpal bones forming the palm. Each metacarpal meets its corresponding finger at the metacarpophalangeal (MCP) joint — the knuckle — allowing flexion, extension and controlled spreading of the fingers.
The fingers consist of phalanges. Most fingers contain three phalanges separated by interphalangeal joints (PIP and DIP joints), functioning as hinge joints to allow bending and straightening.
The thumb is structurally unique. It has only two phalanges and one interphalangeal joint, and it articulates with the wrist at the carpometacarpal (CMC) joint, a saddle joint that permits opposition — a movement fundamental to grip.
It is at the radial side of this complex structure — near the distal radius — that De Quervain’s tenosynovitis develops.
The First Dorsal Compartment
On the thumb side of the wrist, just proximal to the base of the thumb, two important tendons pass through a narrow fibro-osseous tunnel beneath a thickened band of connective tissue called the extensor retinaculum.
These tendons are:
Extensor Pollicis Brevis (EPB):
This muscle extends the thumb at the metacarpophalangeal joint and contributes to thumb positioning during grip. It is active when giving a thumbs-up or stabilising the thumb during lifting.
Abductor Pollicis Longus (APL):
This muscle abducts the thumb — moving it away from the palm — and assists in stabilising the wrist during forceful grip and lifting tasks.
Both tendons share the confined space of the first dorsal compartment, which sits directly over the radial styloid of the distal radius.
Importantly, this compartment is often anatomically variable. Some individuals have a fibrous septum dividing the APL and EPB into separate channels. This can reduce available space and increase friction, predisposing the tendons to irritation.

Tendon Sheath Mechanics
The APL and EPB tendons are encased within a synovial sheath that allows them to glide smoothly during thumb movement.
Every time the thumb:
-
Abducts
-
Extends
-
Stabilises during gripping
-
Assists wrist deviation
These tendons move within the sheath. Because the compartment is narrow and rigid, even mild thickening of the sheath or mild swelling can significantly impair tendon glide.
In early presentations, inflammatory processes may contribute to swelling within the sheath. In more persistent cases, histological studies often demonstrate:
-
Fibrous thickening of the retinaculum
-
Myxoid degeneration
-
Reduced gliding space
Rather than simple acute inflammation. The central problem is therefore mechanical restriction within a confined anatomical tunnel.
Why This Region Is Vulnerable
The thumb is responsible for a large proportion of hand function. During lifting — particularly lifting with the wrist slightly deviated and the thumb abducted — the APL and EPB experience high repetitive loads.
Unlike larger muscle groups, these tendons operate in a tight, non-expanding compartment at the radial styloid. There is limited capacity to accommodate swelling or hypertrophy. When repetitive thumb loading exceeds the capacity of the tendon–sheath system to adapt, friction increases, glide reduces, and symptoms develop.
Clinical History and Symptom Behaviour
De Quervain’s is primarily a clinical diagnosis.
The pattern of symptoms, the location of tenderness, and the response to specific thumb and wrist movements usually provide sufficient clarity without the need for imaging.
However, because pain on the thumb side of the wrist can arise from several structures, careful anatomical reasoning is important.
Clinical History
The history often reveals a gradual onset of pain along the radial side of the wrist. Patients frequently describe discomfort when:
-
Lifting a baby under the arms
-
Gripping or twisting
-
Using a smartphone
-
Performing repetitive thumb-based tasks
The pain is typically localised and mechanical — worse with thumb abduction or wrist deviation, and improved with rest. There is usually no history of significant trauma.
Unlike nerve conditions, sensory disturbance is absent and unlike thumb arthritis, stiffness within the joint itself is not the dominant feature.
Palpation and Localisation
On examination, tenderness is usually highly localised over the first dorsal compartment at the level of the radial styloid.
Patients can often identify the painful point precisely with one finger. Swelling may be present, although it is not universal. Pain is reproduced when the APL and EPB tendons are activated against resistance, particularly with thumb abduction or extension combined with wrist movement.
Finkelstein’s Test vs Eichhoff’s Test
The Finkelstein test is commonly referenced in the diagnosis of De Quervain’s, but it is often performed incorrectly. A true Finkelstein test involves the examiner stabilising the patient’s thumb and gently deviating the wrist ulnarly. When positive, this manoeuvre produces sharp pain directly over the first dorsal compartment.
The Eichhoff manoeuvre — often mistakenly labelled as Finkelstein’s — involves the patient tucking the thumb into the palm and actively deviating the wrist toward the little finger. This version is more forceful and can provoke discomfort even in individuals without pathology.
For that reason, a positive Eichhoff manoeuvre alone does not confirm De Quervain’s. The test must be interpreted alongside localisation of tenderness and symptom pattern.
Provocation without anatomical correlation is not diagnostic.
Differentiating from Thumb CMC Arthritis
Thumb carpometacarpal arthritis is one of the most common alternative causes of radial wrist pain.
In CMC arthritis:
-
Pain is centred at the base of the thumb joint
-
Pinch strength is often reduced
-
There may be crepitus or grinding
-
Joint stiffness is more prominent
The CMC grind test may reproduce joint pain, whereas in De Quervain’s, pain is more superficial and tendon-based.
Accurate localisation is the key distinction.
The Role of Imaging
Imaging is rarely required in straightforward cases.
Ultrasound may demonstrate:
-
Thickening of the tendon sheath
-
Fluid within the compartment
-
Septation
However, imaging findings must correlate with symptoms. Many anatomical variations are asymptomatic. MRI is rarely necessary unless alternative pathology is suspected.
When to Reconsider the Diagnosis
If pain is diffuse rather than localised, if neurological symptoms are present, or if symptoms do not follow a mechanical pattern, alternative diagnoses such as nerve irritation or inflammatory arthropathy should be considered.
De Quervain’s remains a diagnosis grounded in anatomical localisation and reproducible mechanical provocation.
Physical Examination
On examination, maximal tenderness in radial tunnel syndrome is usually located over the radial tunnel itself — typically several centimetres distal to the lateral epicondyle, along the course of the deep branch of the radial nerve.
This contrasts with tennis elbow, where tenderness is usually most focal directly over the lateral epicondyle at the origin of the common extensor tendon. In lateral epicondylitis, patients can often identify the painful point precisely with one finger.
Resisted supination with the elbow extended may reproduce symptoms in radial tunnel syndrome. This manoeuvre increases tension within the supinator muscle and stresses the deep motor branch of the radial nerve as it passes through the radial tunnel. Pain reproduction during resisted supination tends to support neural irritation rather than primary tendon overload.
By contrast, tennis elbow more commonly produces pain with resisted wrist extension, particularly when the wrist is extended against resistance with the elbow straight. The discomfort in that case is typically centred at the tendon origin rather than deeper in the proximal forearm.
The middle finger extension test may also provoke pain in radial tunnel syndrome. This likely reflects increased tension within the extensor-supinator complex and indirect stress on the deep branch of the radial nerve. However, this test can also be positive in tennis elbow, which is why it should not be interpreted in isolation.
Wrist extension strength is usually preserved in radial tunnel syndrome, although pain may inhibit maximal effort. True motor weakness — particularly loss of active finger extension — should not be present in uncomplicated radial tunnel irritation. If objective weakness is detected, especially involving finger extension at the metacarpophalangeal joints, posterior interosseous nerve syndrome must be considered.
This distinction is critical. In tennis elbow, strength is typically preserved and pain-limited. In posterior interosseous nerve compression, weakness is mechanical and not simply pain-related. Radial tunnel syndrome sits between these patterns — pain dominant, without clear motor deficit.
Careful localisation of tenderness and identification of the movement that most consistently reproduces symptoms help determine whether tendon overload, nerve irritation, or a combination of both is the primary driver.
The Role of Nerve Conduction Studies and Imaging
Nerve conduction studies are frequently normal in suspected radial tunnel syndrome. This does not necessarily invalidate the diagnosis.
Unlike fixed entrapment neuropathies, radial tunnel irritation may be dynamic and load-dependent. Compression may occur during movement or under strain but not be severe enough to produce measurable conduction delay at rest.
Imaging is typically unremarkable unless a space-occupying lesion, ganglion, or structural abnormality is present. For most individuals, imaging does not provide decisive diagnostic clarity.
Because objective findings may be subtle or absent, overdiagnosis is possible. A cautious, anatomically informed approach is therefore essential.
Treatment and Management of De Quervain’s Tenosynovitis
Management of De Quervain’s focuses on reducing friction within the first dorsal compartment and restoring smooth tendon gliding.
Because the pathology often involves sheath thickening and restricted movement within a confined anatomical tunnel, the goal is to reduce mechanical compression and allow the tendons to move freely again.
Unlike degenerative tendinopathy, this condition responds well to targeted interventions that reduce compartment pressure.
Activity Modification – Reducing Mechanical Compression
The first step is identifying movements that repeatedly load the APL and EPB tendons under compression. Activities that combine:
-
Thumb abduction
-
Wrist ulnar deviation
-
Forceful gripping
Increase friction within the compartment. Small technique changes can make a substantial difference.
For example:
-
Lifting with the palm up rather than thumb extended
-
Avoiding repetitive one-handed lifting
-
Reducing sustained smartphone thumb use
-
Modifying gym grip position
The aim is not total rest, but reducing repetitive compression in the acute phase.
Splinting – Why It Helps
A thumb spica splint limits excessive thumb movement and reduces mechanical friction within the compartment.
In highly irritable cases, short-term immobilisation allows:
-
Reduced tendon movement
-
Decreased sheath irritation
-
Pain reduction
However, prolonged immobilisation is rarely ideal. The goal is temporary unloading, not dependency.
Splinting is most useful in early or highly reactive presentations.
Progressive Reloading
Once pain settles, gradual reintroduction of movement is important.
Unlike classic tendinopathy where heavy progressive loading is central, De Quervain’s rehabilitation focuses more on restoring smooth tendon glide and balanced thumb control.
This may include:
-
Gentle thumb extension and abduction under low load
-
Wrist stabilisation work
-
Gradual return to functional grip tasks
Complete prolonged rest can reduce tolerance and delay recovery.
Corticosteroid Injection – Why It Works Here
Corticosteroid injection has relatively strong evidence in De Quervain’s compared to many other upper limb tendon conditions.
The reason is anatomical. The pathology often involves thickening and irritation of the tendon sheath within a confined space. Injection into the first dorsal compartment can:
-
Reduce inflammatory mediators
-
Decrease synovial proliferation
-
Reduce swelling within the sheath
-
Improve tendon glide
Because the compartment is small and well-defined, accurate injection often produces significant symptom relief.
Success rates are generally high, particularly when:
-
The injection is delivered precisely into the compartment
-
The anatomical septum (if present) is addressed
In persistent cases, injection may be considered before surgical referral.
This differs from lateral epicondylitis, where steroid injection may offer short-term relief but poorer long-term outcomes.
When Is Surgery Considered?
Surgical release of the first dorsal compartment is highly effective when conservative measures fail.
The procedure involves:
-
Opening the thickened sheath
-
Releasing constrictive tissue
-
Restoring tendon glide
Because the underlying problem is often mechanical restriction, surgical decompression addresses the root cause.
Outcomes are typically very good, particularly when performed for well-defined cases that have not responded to appropriate conservative care.
Recurrence is uncommon when the compartment is fully released.
What Improves Outcomes?
The strongest contributors to recovery are:
-
Early recognition
-
Reducing repetitive compression
-
Avoiding prolonged aggravating activity
-
Appropriate escalation when needed
Unlike degenerative tendon conditions, De Quervain’s often has a clear anatomical driver and therefore responds well to targeted intervention.
Summary
De Quervain’s tenosynovitis is a condition affecting the abductor pollicis longus and extensor pollicis brevis tendons as they pass through the first dorsal compartment on the thumb side of the wrist.
It develops when these tendons become irritated within a confined fibro-osseous tunnel, leading to pain during gripping, lifting, twisting, and repetitive thumb movement. Although often described as an inflammatory condition, many cases involve mechanical thickening of the tendon sheath and reduced gliding space rather than acute inflammation alone.
Accurate localisation of pain is essential. De Quervain’s differs from thumb carpometacarpal arthritis, which produces deeper joint-based pain and stiffness, and from nerve irritation, which would typically cause sensory symptoms.
Most cases respond well to load modification and, where necessary, short-term splinting. Corticosteroid injection has strong evidence in persistent cases because it directly addresses sheath irritation within the compartment. Surgical release is highly effective when conservative treatment fails.
With appropriate management, the prognosis is generally very good.
Educational Notice
This content is intended for educational guidance only and reflects current evidence and clinical reasoning at the time of publication. It does not replace individual assessment, diagnosis, or treatment provided by your healthcare practitioner. Management decisions should always be based on personalised clinical evaluation.
Feel Free To Share
There is a great deal of misinformation and oversimplified advice online regarding musculoskeletal and spinal conditions. If you have found this page helpful, you are very welcome to share it with anyone who may benefit from clear, evidence-informed information.
Please share the page in full via direct link. Reproduction, copying, or republishing of the written content or images without permission is not permitted. Producing accurate educational material of this depth takes significant time, clinical experience, and ongoing review — and I choose to keep it freely accessible for the benefit of patients and healthcare professionals.
Responsible sharing is genuinely appreciated.
Frequently Asked Questions About De Quervain's Tenosynovitis
1) What is De Quervain’s tenosynovitis?
De Quervain’s tenosynovitis is irritation of the abductor pollicis longus and extensor pollicis brevis tendons as they pass through a narrow compartment on the thumb side of the wrist. It causes pain with gripping, lifting, and thumb movement due to restricted tendon glide within the sheath.
2) Where is the pain located in De Quervain’s?
Pain is typically felt along the radial (thumb) side of the wrist, just below the base of the thumb at the level of the radial styloid. It is usually well localised and worsens with thumb abduction or wrist deviation.
3) Is De Quervain’s the same as thumb arthritis?
No. Thumb carpometacarpal (CMC) arthritis affects the joint at the base of the thumb and often causes deeper joint pain, stiffness, and reduced pinch strength.
De Quervain’s affects the tendon sheath and causes pain slightly more superficial and along the tendon path rather than within the joint itself.
4) Why is De Quervain’s common after pregnancy?
De Quervain’s is frequently seen in the post-partum period. Repetitive lifting of an infant combined with hormonal and fluid changes may increase tendon sheath sensitivity. The repetitive thumb-abducted lifting position places sustained load on the first dorsal compartment.
5) What is the Finkelstein test?
The Finkelstein test is a clinical manoeuvre used to assess for De Quervain’s. When performed correctly and gently, it reproduces pain over the first dorsal compartment by stressing the involved tendons.
A more forceful variation (Eichhoff’s test) can provoke pain even in normal wrists and must be interpreted carefully.
6) Does De Quervain’s involve inflammation?
In early stages, inflammation may contribute. However, many persistent cases involve thickening of the tendon sheath and mechanical restriction rather than pure inflammatory swelling.
This is why reducing friction within the compartment is central to treatment.
7) How long does De Quervain’s take to heal?
Mild cases may settle within weeks if aggravating activities are reduced. More persistent cases can last several months if repetitive thumb loading continues.
With appropriate management, the prognosis is generally very good.
8) Does a wrist splint help De Quervain’s?
A thumb spica splint can help in more irritable cases by limiting thumb movement and reducing friction within the tendon sheath. It is usually used short-term rather than indefinitely.
9) Are steroid injections effective for De Quervain’s?
Yes. Corticosteroid injection into the first dorsal compartment has strong evidence of effectiveness. It reduces sheath inflammation and swelling, often providing significant symptom relief, particularly when delivered accurately.
10) When is surgery needed for De Quervain’s?
Surgery is considered when symptoms persist despite appropriate conservative treatment and, in some cases, injection therapy. The procedure involves releasing the tight sheath to restore tendon glide. Outcomes are typically very good.
Why You Should Choose Chris Heywood Physio
The most important thing when seeking help is finding a practitioner you trust—someone who is honest, responsible, and clear about your diagnosis, the treatment you really need, and whether any follow-up appointments are necessary.
I’m not here to poach you from another therapist, but if you’re looking for a new physiotherapist in Northamptonshire or simply want a second opinion, here’s why many people choose to work with me (read my reviews):
Over 25 Years of Experience & Proven Expertise
With 25+ years of hands-on physiotherapy experience, I’ve built a trusted reputation for clinical excellence and evidence-based care. My approach combines proven techniques with the latest research, so you can feel confident you’re in safe, skilled hands.
Longer Appointments for Better Results
No two people—or injuries—are the same. That’s why I offer 60-minute one-to-one sessions, giving us time to:
-
Thoroughly assess your condition
-
Provide focused, effective treatment
-
Explain what’s really going on in a clear, simple way
Your treatment plan is tailored specifically to you, aiming for long-term results, not just temporary relief.
Honest Advice & Support You Can Trust
I’ll always tell you what’s best for you—even if that means you need fewer sessions, not more. My goal is your recovery and wellbeing, not keeping you coming back unnecessarily. I have low overheads nowadays and I do not have pre-set management targets to maximise patient 'average session per condition' (yes it does happen commonly and I hate it with a passion - read my article here)
Helping You Take Control of Your Recovery
I believe the best outcomes happen when you understand your body. I’ll explain your condition clearly, give you practical tools for self-management, and step in with expert hands-on treatment when it’s genuinely needed.
Looking for a physiotherapist who values honesty, expertise, and your long-term health?
Book an appointment today and take the first step towards feeling better.
Contact Info
On a Monday and Tuesday I work as a advance musculoskeletal specialist in primary care but I can still be contacted for enquiries. You are welcome to call but it is often faster for me to reply via an email or watsapp message, simply as my phone will be on silent in clinic. Either way, I will reply as soon as possible, which in the week, is almost always on the same day at the latest.

Clinic Opening Hours
** Please note that online sessions and Aquatic sessions be arranged outside of normal clinical hours on request.**
Sat -Sun
Closed
0900 - 1430
Closed - FCP
Weds - Fri
Mon - Tues










